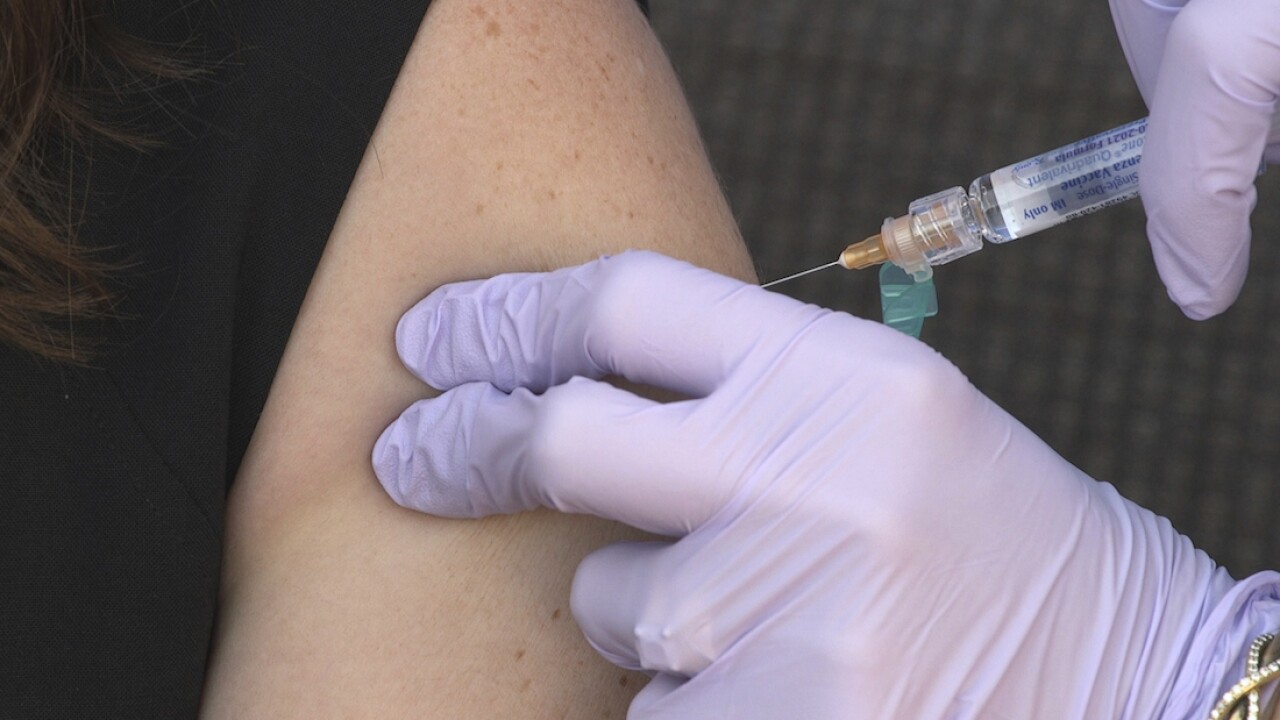
LAS VEGAS (KTNV) — On Thursday, the Centers for Disease Control and Prevention abruptly announced new guidance on mask-wearing, saying Americans who are fully vaccinated no longer need to wear them in most cases, including indoors.
Following this announcement, 13 Action News spoke with Dr. Domenic Martinello, the Chief Medical Officer at Southern Hills Hospital, to clear up any remaining COVID-19 vaccine confusion.
13 Action News asked Dr. Martinello the following questions and got the following answers.
Q: If you have been vaccinated against COVID-19, can you still contract the virus? If so, what is the likelihood?
A: "Your likelihood of contracting the virus after being fully vaccinated depends on which vaccine you received. So for the two predominant ones, the Pfizer and the Moderna vaccine, we know that they're greater than 90% effective at preventing what they call, 'symptomatic infection.' In terms of actually being able to contract the virus, if you're exposed to it and it gets into your body, that doesn't necessarily mean that you're going to get the disease. Your immune system will fight it off rather briskly afterwards. So in terms of being symptomatic, it's greater than 90% effective. And it's also much more effective in preventing what they call, 'severe disease,' meaning hospitalization, and even more effective with preventing death. Nothing is 100%. Not everybody's immune system responds exactly the same. There are some people who may have weakened immune systems. There are some people who may just be unlucky and their body doesn't fight it off quite quick enough. But the reality is, with the vaccines, the effectiveness is high enough that that's the only way that we're ever going to get to what they call, 'herd immunity, or enough immunity in our population to prevent spread. So if you combine somewhere between 90%-95% efficacy of a vaccine, mixed with a large portion of the population who has it, now you have decreased transmission, decreased deaths, decreased risk of people even getting sick and doing something as simple as missing work. And then, eventually you get what they call 'viral control,' where you have such low levels of it that these things may become locally epidemic but not pandemic, meaning global," said Dr. Martinello.
Q: If the vaccines don't provide 100% protection against COVID-19, why bother getting them?
A: A pandemic like this is incredibly transmissible. If you look at the R0, which is kind of the measure of infectivity, it's somewhere in the order of three, which means every person that gets infected will infect approximately three other people. That's extremely contagious. And the only way that we're gonna get past that is through vaccination. If you want to look at mortality, COVID-19 has about a 1% mortality compared to the vaccine, which we haven't seen direct, high levels of mortality from. We're looking at orders of one in a million, compared to one in 100. Going even deeper into those numbers, you have to consider things other than mortality, which is what we call morbidity from from the disease. So the COVID-19 disease seems to cause a lot of blood clotting, which has caused young and otherwise healthy people to have heart attacks, strokes. We've seen people with permanent lung injury, permanent cardiac injury, brain injury. So if you even look deeper than that 1% of people who would die, we're looking at large numbers of people who have permanent life-altering changes because of this disease. If you compare that to the risk of getting a vaccine, which is extremely small, you can see why the vaccine is just a better alternative.
Q: If you have been vaccinated against COVID-19, can you still spread the virus to others?
A: "Vaccines are very effective at producing immunoglobulins in the body, which is how they work. You have these immunoglobulins that float around, they bind to a virus. One of the ones that the vaccine doesn't really create very well is what they call IgA, which is predominant in the nasal passages and in the mouth and throat and the GI tract. So the idea is that you can actually be locally infected in the nasal region or in the mouth, and still able to spread it. And in the recent studies, they noted transmissibility was cut about in half for people who are vaccinated, meaning if you take that R0 of three and you make that an R0 of one and a half, or if you're normally going to infect three people you'd only infect one or two. And then you have to think in order of magnitude. If all of those people were also vaccinated, that decreases the spread as well. So although you are still capable of spreading it, you've cut that about in half in most studies. Now if you couple that with, if you're vaccinated and the person that you're around is vaccinated, if one of you has it, you all you have a 50% chance that you could spread it, but you also have a vaccinated person who's 90% likely to fight it off or not get sick from it at all. So, again, the idea is that from an individual level, it's about 50%, it cuts the risk about in half. But on the other side, if everybody's vaccinated, their risk is also cut down significantly," said Dr. Martinello.
RELATED: COVID-19 Vaccines and What You Need To Know
Q: Will wearing a mask reduce the risk of this vaccinated spread?
A: "There's certainly a benefit. I mean, the mask mandates come around from a public health preventative standpoint. If you really want to prevent spread, you have to use all measures at hand, which includes vaccination, social distancing, mask-wearing. The reason that the mask mandates are slowly being taken back now is because the amount of local disease is finally getting low enough that the risk is getting low. And once the risk gets below a certain threshold, which is typically somewhere between 5%-7%, you start to be able to relax some of these measures. Now, if those measures result in the population becoming more infectious, those would certainly need to go back in place. The biggest risk, of course, is when people start thinking, 'okay, these are being loosened slightly,' and then people kind of open the floodgates. We don't want to just have a lot of people in close confines indoors without masks. What we want are vaccinated people who are at low risk to be able to relax some of these restrictions, especially outdoors, where the risk of transmission is already slightly lower. You add in mass vaccination, a population that has a low rate of transmissibility, and you can get to this point where we start returning to normal," said Dr. Martinello.
Q: If you've been diagnosed with COVID-19 before, should you still get the vaccine? Why or why not?
A: In the short term, they do have some immunity, which we call natural immunity. The unfortunate part of that is that typically you develop kind of short-lived antibodies to one very specific virus. When you look studies, the people who had COVID and then were exposed to some of these variants, a large number of them still got infected by the variants. One of the problems is that you don't produce the immunoglobulin reliably or to specific sources. One person may have a nucleocapsid antibody, another person may produce an antibody to a spike protein, whereas with the vaccines, you're producing a very specific antibody to a very specific target which is these conserved regions of the spike protein. And that's why we're seeing the vaccine being effective against the vast majority of these variants as well, compared to natural immunity where you may or may not develop immunity to the South Africa variant or the UK variant. And it's even more important, for that reason, that people who have had COVID go out and get vaccinated. And if you haven't had COVID, go out and get vaccinated," said Dr. Martinello.